The term herd immunity comes from the observation of how a herd of buffalo forms a circle, with the strong on the outside protecting the weaker and more vulnerable on the inside.
This is similar to how herd immunity works in preventing the spread of infectious diseases. Those who are strong enough to get vaccinated directly protect themselves from infection. They also indirectly shield vulnerable people who cannot be vaccinated.
There are various reasons a person may not be able to be successfully vaccinated. People undergoing cancer treatment, and whose immune systems are compromised, for instance, are impaired in their ability to develop protective immunity from all vaccines. Often, people who can’t be vaccinated are susceptible to the most serious consequences from being infected.
Another vulnerable group are babies. Infants under six months of age are susceptible to serious complications from influenza. Yet they can’t be given the flu vaccine as their immune systems are not strong enough.
How does herd immunity work?
For a contagious disease to spread, an infectious agent needs to find susceptible (non-immune) people to infect. If it can’t, the chain of infection is interrupted and the amount of disease in the population reduces.
Another way of thinking about it is that the disease needs susceptible victims to survive in the population. Without these, it effectively starves and dies out.
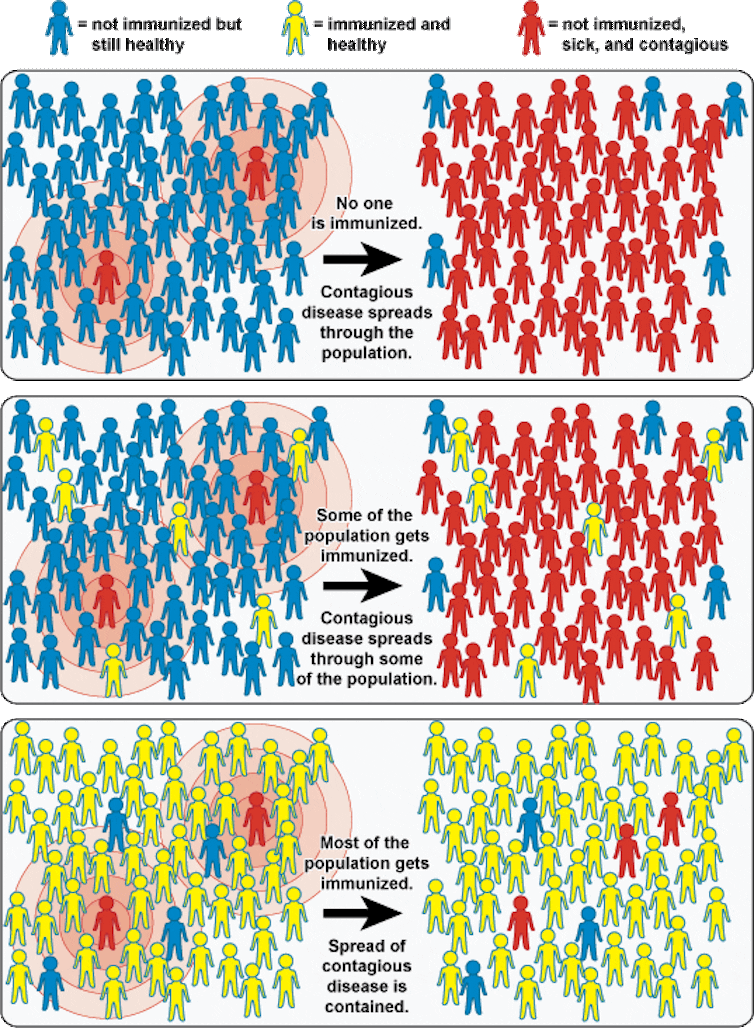 If most of the population is immunised, the disease dies out (Photo:
If most of the population is immunised, the disease dies out (Photo:
NIAID, CC BY)
What level of coverage provides herd immunity?
How many people need to be vaccinated to achieve herd immunity varies from disease to disease.
Measles can be transmitted through coughing and sneezing and the virus causing measles can survive outside the body for up to two hours. So it’s possible to catch measles just by being in the same room as someone who is ill if you touch a surface they’ve coughed or sneezed on.
In contrast, Ebola can only be spread by direct contact with infected secretions (blood, faeces or vomit) and therefore requires close contact with an ill person. This makes it much less spreadable.
We can determine how contagious a disease is by tracking its spread throughout a population. In doing so, we can attribute each disease a reproductive number denoted by the symbol Ro. The bigger the Ro the more easily the disease is spread throughout the population.
If everyone who has a disease on average infects two people, the Ro for that disease is 2. This means the disease, relatively speaking, is not particularly contagious. However, if everyone who has a disease infects ten people on average, it would have an Ro of 10, which means it’s a much more contagious disease.
We can use the Ro for a disease to calculate the herd immunity threshold, which is the minimum percentage of people in the population that would need to be vaccinated to ensure a disease does not persist in the population. The more contagious a disease, the higher the threshold.
Measles is one of the most infectious diseases to affect humans with an Ro of 12-18. To achieve herd immunity to measles in a population we need 92-95% of the population to be vaccinated.
Current data indicates full vaccine coverage for five year olds in Australia is sitting at around the 95% level. However, vaccination rates in some communities have fallen below ideal levels, making them susceptible to measles outbreaks.
The overwhelming success of measles vaccinations means many people have no memory of what this disease looks like, and this has resulted in its effects being underestimated. Measles can cause blindness and acute encephalitis (inflammation of the brain), which can result in permanent brain damage.
Herd immunity, or community immunity, as it’s sometimes called, is a powerful public health tool. By ensuring those who can be vaccinated do get vaccinated we can achieve herd immunity and prevent the illness and suffering that comes from the spread of infectious diseases.
Hassan Vally, Associate Professor, La Trobe University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Get the latest from The Adelaide Review in your inbox
Get the latest from The Adelaide Review in your inbox